Last Updated on December 19, 2024 by The Young Firm
In maritime work, some injuries are more common than others. As a result, there are certain common medical diagnostic tests doctors use to examine injured maritime workers. If the company doctor refuses to give you an MRI or an X-ray (the most basic of medical tests), then you’ll need a second opinion on your injury. The company doctor may not have your best interests at heart.
If you’re currently seeing a company doctor, make sure they perform pertinent medical tests to fully explore your injury. Here is a list of medical tests commonly performed on injuries:
- Magnetic Resonance Imaging Scan (MRI)
- X-ray
- CT scan
- Discogram/Myelogram.
- Arthroscopic surgery
- Electromyogram (EMG)
- Epidural Injections
- Sympathetic Block
What is a Magnetic Resonance Imaging (MRI)?
A magnetic resonance imaging scan (MRI) is one of the most common tests performed to diagnose most injuries to a neck, back, shoulder or knee. An MRI scan shows soft tissue and ligament damage and provides a more detailed view than a CT scan. It’s generally a good idea to get an MRI roughly a week or so after the injury since many soft tissue injuries won’t show up immediately.
MRIs diagnose damaged lumbar and cervical discs, and torn ligaments. If you have suffered any type of injury that has bothered you for more than a few days, it is best to get an MRI scan. Many company doctors will delay performing an MRI since they may not want to charge your company for the expense. It is important that you insist that all medical testing be performed, including MRIs. The more traditional MRI is performed in a long tube. There is also a more advanced type of MRI known as a “stand-up” MRI scan, which is taken while the patient is standing. Very often, this can more accurately reflect any type of herniated or damaged lumbar or cervical discs. This is because the scan is taken while the patient is actually placing weight on their lower back and neck.
What is an X-ray?
An X-ray is a basic imaging scan of an individual’s bones. An X-ray does not show soft tissue or ligament/tendon damage, nor will it indicate nerve damage.
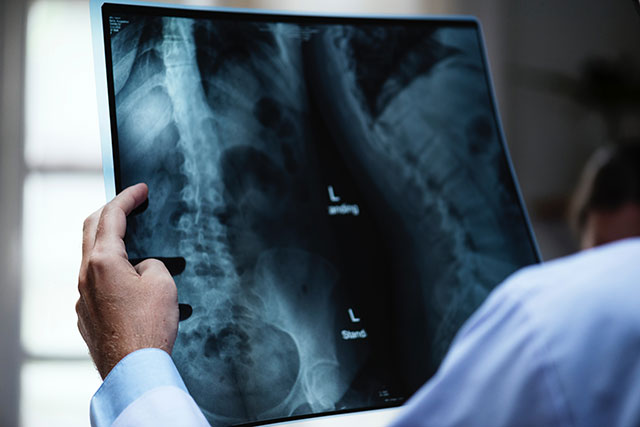
Most doctors and health facilities will immediately perform an X-ray following an injury. It is very important to understand that X-rays will not diagnose the majority of serious injuries.
X-rays DO NOT reveal:
- Ligament/tendon damage
- Nerve damage
- Lumbar disc injuries
- Joint damage
These types of injuries need to be diagnosed with other tests, including MRIs, CT scans and nerve conduction studies.
What is a CT Scan?
A CT scan (also called a CAT scan) is a form of enhanced X-ray that can diagnose soft tissue, organ and blood vessel type injuries. Often, a CT scan will be performed after an MRI scan to further diagnose or investigate the individual’s injury. The most helpful CT scans are usually performed “with contrast.” This means that the individual will drink (or have IV injected) a specialized dye before the CT scan is performed. The dye allows the CT scan to give a much more accurate, detailed image of the injured area.
What is a Discogram/Myelogram?
A discogram is a procedure during which dye is injected into a person’s cervical or lumbar discs. The purpose of the test is to determine if the injected dye leaks out or goes beyond the subject disc. A discogram can be a very accurate way to determine the full extent of a person’s injury.
Healthy lumbar and cervical discs will hold the small amount of dye that is injected. This is because a normal, healthy disc is fully enclosed and encapsulated. If a lumbar or cervical disc has been injured, this will often result in a tear in the disc. When a small amount of dye is injected into the disc, it will immediately leak out, indicating that the disc has a hole or tear in it.
A discogram is often followed by a CT scan which will take images of the disc and the dye in order to see if the dye has moved outside of the disc. A myelogram is very similar to a discogram in that dye is injected around the injured (typically) lumbar or cervical area. A CT scan is then performed to view the area, and the dye provides an enhanced image of any damage to that area.
What is Arthroscopic Surgery?
Although arthroscopic surgery is considered a “surgical” procedure, it is often used to diagnose injuries that may not be visible with other non-invasive tests. Orthopedists typically perform arthroscopic surgery on an individual’s knee and shoulder areas. The purpose of this surgery repairs any damage which may be seen, and helps visualize damage which may not have appeared on prior MRI and CT testing.
What is an Electromyogram (EMG) and Nerve Conduction Study (NCS)?
An electromyogram (EMG) is a test that is used to record the electrical activity of muscles. When muscles are active, they produce an electrical current. An EMG is usually given at the same time as a nerve conduction study. The most common type of nerve conduction study is known as a nerve conduction velocity (NCV) test. These tests are used to diagnose nerve injuries and muscle damage.
Often, they will be given to individuals who have suffered lower back injuries or neck injuries to diagnose nerve damage that may be occurring in the person’s upper or lower extremities (arms or legs). The NCV will measure how quickly and completely a person’s arm or leg nerve transfers “information,” or how quickly and completely they respond. If nerve damage has occurred very often, the response will be delayed or incomplete.
It is very important to note that most EMG/NCV tests are not 100% accurate. Most physicians will admit that the tests have at least a 10% margin of error. Often, individuals with nerve damage will have normal EMG/NCV tests even though they are experiencing nerve damage.
What are Lumbar Epidural Steroid Injections?
Lumbar epidural steroid injections (also known as epidural injections or steroid injections) is a series of injections typically given in a person’s neck or lower back in an attempt to relieve pain from a damaged cervical or lumbar disc. Epidural injections can also be given in an individual’s shoulder area as well as other parts of the body.
Epidural injections are often described as both therapeutic and diagnostic. This means the injection is given to provide relief to the patient as well as potentially diagnose their injury. Most doctors believe that if the patient receives temporary relief for a period of days or even a few weeks from the injection, this means that the injection was most likely given at the source of the injury. In this way, the injection serves as a diagnostic tool to help the doctor identify the area of injury.
What is a Sympathetic Block?
A sympathetic block is a type of test that is performed as both a treatment and diagnostic. A sympathetic block is given to a patient to diagnose nerve damage typically into their lower legs, feet or ankles. The basic purpose of the sympathetic block is to prevent” the nerve communication from the suspected injury to the person’s brain.
If the sympathetic block is successful, the person will receive relief since the injured part of the body temporarily will not communicate with the individual’s brain. This result indicates to the doctor that the person is suffering from nerve damage at the point of the injury. If the sympathetic block is successful (and very often a series of them are performed), the doctor may consider permanently “disconnecting” that nerve such that it will no longer send messages of pain to the person’s brain.
All these procedures can help doctors focus on your injury and help diagnose causes. Getting the right tests will help your health and your case.
Contact Us With Any Questions About Your Maritime Injuries
At The Young Firm, we are focused on Jones Act and maritime injury law cases, and we understand claims like yours because we have handled so many of them. We are well aware of the specific requirements that victims of maritime accidents have, and we can help you recover your lost benefits and get you compensation for damages.
Schedule your free consultation today! If you have questions about maritime injuries and how to receive fair compensation, contact a lawyer from The Young Firm at 504-680-4100.
Other articles about medical procedures and best practices:
